It’s too bright in here.
No. No, no, no, no, no. I don’t want this.
WHAT is that? They didn’t tell me about that.
I don’t want it, I don’t want it. I want to get up.
No. NO.
I’m going to be sick. I AM GOING TO BE SICK. Can’t you hear me?
I don’t have to calm down, this is wrong, I don’t want to be here.
No. No I don’t need this, I don’t want this.
Let me up. LET ME UP.
I’m going to be sick, again. AGAIN.
Morphine?
I don’t want to be here.
It’s too bright.
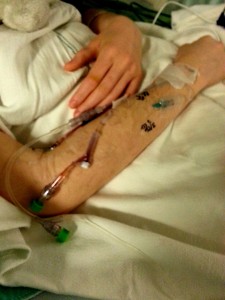
I’m told I didn’t wake up in the Post-Anesthesia Care Unit (PACU) with grace. I think perhaps luckily, I don’t remember the majority of the experience. What I remember most about waking up following 12 hours of brain surgery to remove an acoustic neuroma (more than 14 hours away from my family) is being angry that I was hooked to so many devices. I had three IV needles (though only one was in action), a catheter, a plastic bulb connected to an incision in my belly button collecting fluid, a heart monitor with five attachment points, and I couldn’t move my head because I had a heavy bandage wrapped around my brain like a donut. I woke up angry, and I woke up confused, and I woke up feeling, as I apparently slurred at my family, “aaawwfullllll.”
I was angry and confused. Either it was not explained to me, or I never processed the fact that I would have a catheter. Why this horrified me to the level that it did, I’m not sure. The sense of helplessness I guess. How suddenly and unexpectedly I had been transformed from an able-bodied 26-year-old, to unable to exert any control over even the most basic functions of my body made me confused. I wasn’t prepared to wake up in this new reality. I think, “will you put a catheter in me while I’m under anesthesia,” is something I should have asked when the doctors repeatedly beseeched me, “do you have any questions.” But, I didn’t think to ask. Even though it is obvious that I would need one, I hadn’t considered it. I hadn’t considered it because it didn’t even register as something to consider. I didn’t know that I didn’t know.
When I woke up connected to bags and tubes and needles late Thursday night I flipped out. My lack of grace included struggling to sit up, arguing that I didn’t need a catheter, and poking at the bulb collecting fluid, while repeatedly vomiting (into my oxygen mask at one point) before an increased cocktail of sedatives and painkillers finally took the fight out of me. At that point, though I don’t remember my Mom being there, she assures me I vomited on her too. Less than 48 hours before, I thought I would have surgery perhaps in a month. I thought I would go back to work for a while. I thought I had time to get ready for this.
Progressing too quickly
Only a week before I channeled Linda Blair from The Exorcist in the PACU, I was diagnosed with an acoustic neuroma. My diagnosis followed months of symptoms like headaches, dizziness, vertigo, hearing loss, ringing in my ear and numbness in my tongue. It was a long process to get an accurate diagnosis, and I had been assured that my type of tumor was slow growing. My doctors told me to take time to plan for my life to be disrupted by the surgery and recovery. These same doctors warned me to pay attention to the feeling in my face. The numbness I was experiencing in my tongue may just have been a starting point, so, if any other numbness occurred, my medical team needed to know. It could be a sign that the tumor was growing faster than anticipated, a sign that it wasn’t benign after all. If my doctors were going to save my ability to control and feel my face, it was important that there be as little preexisting nerve damage as possible. A week after being diagnosed, I woke up unable to feel half of my face. I was numb from cheek to chin on my right side. Not wanting to be alone, I did what made sense to me, and I went into the office.
I called the doctor too of course, and left a message with the patient coordinator about my new symptom. While I waited to hear from my phsicians, I worked. I tried to answer emails, and tie up some loose ends to square things away. My doctor asked me to come in to see her that afternoon, so in the spirit of “just in case,” I set my out of office message. A friend picked me up and drove me to my appointment. My doctor explained that she felt we needed to get the tumor out as soon as possible, that we really couldn’t wait because my symptoms were worsening at a worrying rate. “Tomorrow,” she said. Tomorrow? I should probably call my parents, huh?
I won’t even begin to speculate what this entire process has been like for my parents. I know calling my Dad to tell him that I needed brain surgery the next day was not easy, so I can’t imagine what it was like on the other end. Luckily, we had already decided what type of surgery I would have, and had been able to meet the surgeons. So, while my parents and my brother rushed from New Jersey to Boston, I was admitted to the hospital. My friend and I walked right from my doctor’s office into the emergency department and explained that I needed to be admitted. My boyfriend joined us, and the three of us switched from the emergency department to a room across the street by ambulance, then back across the street again by ambulance to a different room. I kept offering to walk, but rules are rules and I wasn’t allowed. Of course, I was rewarded for following the rules by losing my shoes during the room switching.
By now Wednesday afternoon had faded into Wednesday night. Things had moved so quickly I hadn’t had time to think about the reality of what was about to happen to me, to my brain, or to my life.
The Procedure
I left my friend and boyfriend sitting in my hospital room so I could get a pre-op MRI. I don’t have a problem with closed spaces, or noise, and I’d been fine during an MRI the week before to diagnose the tumor. So, when my nurse asked me if I needed anything to help me stay calm, I told her no. This was a mistake.
I didn’t really anticipate how LONG I needed to be in the MRI, because the one I’d had a week earlier lasted only 45 minutes. I also overestimated the strength of my emotional state. This time, the technicians needed to take pictures of the tumor to make sure it hadn’t grown. Then they also needed to image my entire spine to make sure there were no additional tumors. I was in the MRI for two hours. Alone. With my brain. My broken brain.
They tell you to hold as still as you can, but I sobbed for the entire last half hour. After the tumor was out, during a follow-up scan, one of the technicians told me that I was “a legend down here” for what had apparently been an out-of-the-ordinary, marathon, late night session.
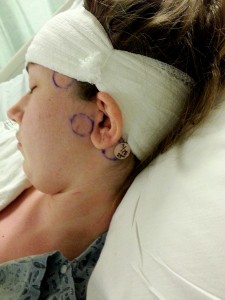
Adding insult to injury, when I finished the MRI, the technicians placed garish glow-in-the-dark stickers, ringed in dark marker on my face. These stickers would serve as a map for the machines the next day, but that night I looked like someone stuck Lifesavers to my forehead.
When they wheeled me back to my room, I was still crying nonsensically and apologizing to absolutely everyone for losing my shit. This is how I entered into the first meeting between my family who had arrived from New Jersey and my new boyfriend, because, on top of brain surgery imploding any sense of normalcy in our lives, dating is still one of life’s most awkward rituals.
I eventually calmed down and tried to sleep, which anyone who has ever spent time in the hospital knows is not easy. It was morning and surgery time in the blink of an eye. They transferred me to the pre-op clinic, where both of my surgeons (one an ear, nose, and throat specialist and one a neuro specialist) came and talked to me. They ran through the procedure. They initialed the parts of my body they intended to cut. They explained the risks, all the things that could go wrong. I spoke to two anesthesiologists. I spoke to my nurse. I signed the consent forms. Everyone asked if I had questions – I did, I just didn’t know it, so I asked nothing. I gave my family a goodbye hug, and was wheeled away.
The last thing I remember is seeing one of my surgeons, and being asked questions – Who am I? Where am I? What day is it? Why am I there? Then there is nothing until I came to in the PACU, confused, upset, and angry.
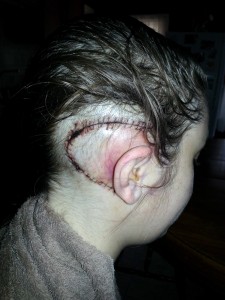
I’ve been actively not thinking about the reality of the surgical procedure itself, because it is overwhelming to think that multiple people have literally seen my brain. My surgeons cut through the bone behind my right ear, and, because their approach cut a nerve completely, they destroyed my ability to hear on this side. This means I’m now deaf in my right ear. Part of the surgery involved packing the hole in my skull with fat taken from my belly button. This is what made the bulb at my abdomen to collect fluid necessary.
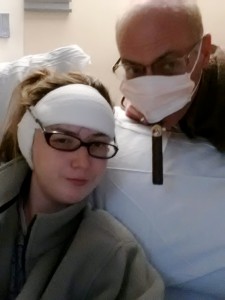
My Dad and I taking a hospital selfie. I was rocking the taped on glasses, him the mask and, yes, that is a cigar.
My family had been told it would be an all day surgery, but it took far longer than anticipated. One of the things the doctors had warned me might go wrong – “stickiness” of the tumor – did. The tumor was clinging to my brain, refusing to let go so easily. So my surgeons took extra time, ultimately clocking in at 12 hours after teasing out every piece. But they got it all, and were able to save my seventh nerve and thus my ability to control and feel my face. While there is no such thing as an ideal brain tumor surgery, my team got it all and avoided any damage to my facial nerves.
I think the decision to move quickly on the surgery was the right one, but it definitely didn’t give me time to process what was happening. I’m certain that contributed to my performance in the PACU. I woke up in a completely new reality that I wasn’t prepared to face. Toward the end of the day on Friday, my memories of the PACU become a little more solid. Apparently, I kicked off my hospital socks as part of my defiant outburst, and I remember being told I had the nicest feet there, which is amazingly awkward upon recollection. I remember my Mom and Dad being there. I remember feeling like the world was spinning. I remember hating the lights. I remember wanting to sleep, which I did a lot.
Recovery
Late Friday night they moved me from the PACU to the Neurosciences floor. Saturday is a bit of a blur too, but I was definitely more with it than I was in the PACU. There were visitors and flowers mixed in among the vitals checks, finger sticks, and medications. Even though I was still hooked to the IV, they took away the catheter, the bulb at my belly button and the heart monitor. That helped a lot. I started to focus more on the donut around my head.
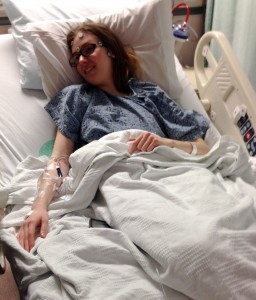
My hair was up in a knot, Pebbles Flintstone style, with a bandage wrapping around my head. There was a hard plastic piece over my right ear wrapped in more bandages. It was heavy. I felt like a bobble head anytime I tried to move, a sensation definitely aided by the fact that my vertigo was intense. My doctors warned me that the vertigo wasn’t going to go away with the surgery and was likely to get worse before it got better: they were right. I also struggled with my vision for the first few days after surgery. I had a hard time focusing and found things to be more blurry with my contacts in than my glasses. Combine my need for glasses with the bandage around my head, and I had a problem, thus I spent my hospital stay with glasses taped to my face.
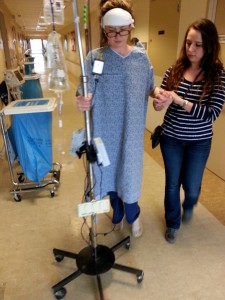
I spent a week in the hospital following the procedure, which was an interesting experience in its own right. I had a constant stream of visitors, and was never alone, which helped tremendously to keep my spirits up. I fully utilized my ability to request quiet time for everyone so I could drop off for a nap. Soon I itched to get out of bed and walk, and I was surprised at how difficult it had become. Since my sense of balance was damaged, I wobbled and lurched around like I had consumed a few too many beers. I put my visitors to work, helping keep me upright, while I leaned on my IV pole and walked up and down the hallway in my slipper socks.
Hospitals themselves are ironically not restful places, particularly the neuro floor. The beds are pressure sensitive, so the nurses can tell if patients are getting up on their own when they aren’t supposed to be. Apparently this happens all the time, prompting a stream of running feet as nurses rush to make sure no one falls over. Getting woken up every four hours for a vitals check, and finger sticks to check my insulin levels wasn’t conducive to sleep either. With the bandage on my head I was unable to shower. After a week in the hospital, this was not exactly pretty, though I tried my best to clean up and feel normal (never really successful, but I tried.)
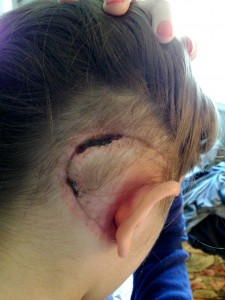
A week after the surgery, they removed the bandage and I was cleared to leave. The vertigo continued intensely, and traveling even the short distance between the hospital and my apartment was rough. I spent a week at my apartment in Boston with my Mom taking care of me. I was still having trouble walking around without tipping over, and I was unable to do things like wash my own hair. I napped a lot, but everyday spent more hours awake and more time on my feet.
Friday April 11, my stitches came out. As I celebrated this milestone, I frustratingly also developed a seroma, a build-up of fluid around my belly button incision. I found out this is also a common complication from liposuction. The sudden onset of swelling was really unnerving, but my doctors answered my phone calls late on a Friday night to set my mind at ease. I can’t say enough good things about my doctors. What times we live in when you can text a surgeon a picture of your belly at 10:30pm on a Friday and get a helpful, calming response.
Even with this complication, my doctors have said they are happy with my progress. I know it will be a long time before I can say I feel like myself, but that is the goal I am working toward.
I can totally relate to your freakout in the PACU. When I woke up after gall-bladder surgery, I was shocked at how badly my stomach hurt. I knew that having someone cut into my body would be painful, but I was having emergency surgery to fix something that was horribly wrong and was emotionally unprepared to hurt more after surgery than I did before.
Part of me wished someone had told me how painful it would be, but I know that I would either have not grasped the magnitude of the hurt or have been frightened going into surgery. There’s no winning here. Needing surgery is a terrible thing, but I am glad yours went well and that you are on your way to recovery. Thank you for writing this very honest and visceral account of your experience.